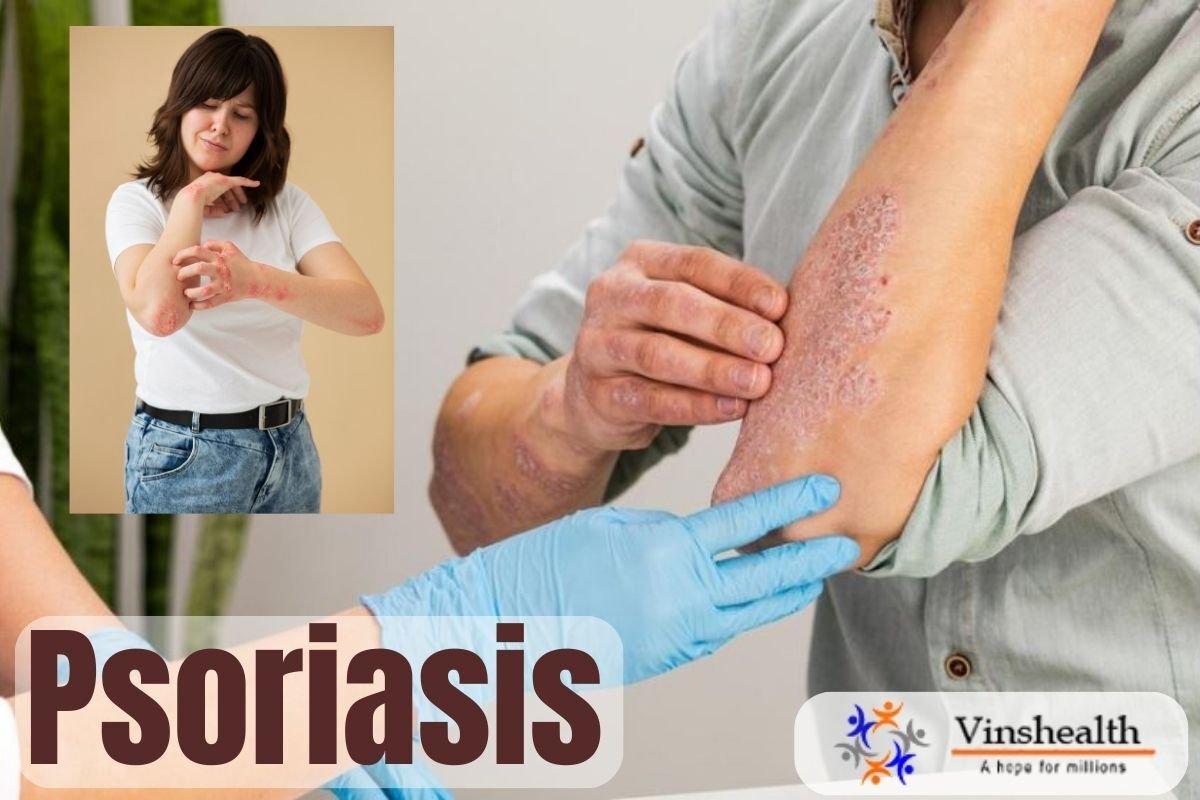
Psoriasis: Causes, Symptoms and Treatment
In the realm of dermatological conditions, psoriasis stands as one of the most complex and enigmatic diseases. Characterized by its distinct appearance on the skin and its often persistent nature, psoriasis affects millions of people worldwide. This blog will delve into the depths of psoriasis, shedding light on psoriasis meaning, psoriasis symptoms, psoriasis causes, and available psoriasis treatment options.
Table Of Content
- What is Psoriasis?
- Psoriasis Symptoms
- Causes of Psoriasis
- Psoriasis Treatment
- Psoriasis Treatment Creams
- Cost of Psoriasis Treatment in India
- The Emotional Impact
- Frequently Asked Questions (Psoriasis)
What is Psoriasis?
Psoriasis is a chronic autoimmune disorder that primarily affects the skin, leading to the rapid buildup of skin cells. This excessive cell growth results in the formation of raised, red, and often scaly patches on the skin's surface. These patches, known as plaques, can be itchy, painful, and even crack and bleed in severe cases. Psoriasis is not contagious, but its visible symptoms can be emotionally distressing for those who experience them.
Psoriasis Symptoms
Psoriasis Symptoms can vary widely from person to person and even in the same individual over time. The most common psoriasis symptoms include:
Plaques: The hallmark of psoriasis, plaques are thick, red patches covered with silvery scales. They can appear anywhere on the body but are most often found on the elbows, knees, scalp, lower back, and face.
Itching and Pain: Psoriasis patches can be intensely itchy and cause discomfort or pain, particularly when they crack and bleed.
Nail Changes: Psoriasis has the potential to impact the nails, resulting in the development of pits, changes in color, and even detachment from the nail bed.
Joint Pain: In some cases, psoriasis is associated with psoriatic arthritis, a condition that causes joint pain, stiffness, and swelling.
Scalp Psoriasis: This variant affects the scalp, leading to red patches covered with silvery scales. It can cause itching and dandruff-like flakes.
Inverse Psoriasis: Commonly found in skinfolds like the armpits, groin, and under the breasts, this type appears as smooth, red lesions that are worsened by friction and sweating.
Causes of Psoriasis
The exact cause of psoriasis is still a subject of ongoing research, but it is widely believed to result from a combination of genetic, immune system, and environmental factors.
Genetics: Having a family history of psoriasis elevates the likelihood of developing the condition. Certain genes related to the immune system have been identified as potential contributors.
Immune System: Psoriasis is an autoimmune disease, meaning the immune system mistakenly attacks healthy cells. In psoriasis, immune cells called T cells become overactive and trigger inflammation, leading to the rapid skin cell turnover.
Triggers: Environmental factors such as infections, stress, injury to the skin (the Koebner phenomenon), and certain medications can trigger or worsen psoriasis symptoms in genetically predisposed individuals.
Lifestyle: Lifestyle factors like smoking, excessive alcohol consumption, and obesity have been associated with a higher risk of developing psoriasis or exacerbating its symptoms.
Psoriasis Treatment
While psoriasis has no known cure, a range of psoriasis treatment options can effectively manage its symptoms and improve the quality of life for those affected. Psoriasis treatment strategies are often tailored to the severity of the condition, its location, and the individual's response to various therapies.
Topical Treatments: These include creams, ointments, lotions, and shampoos containing corticosteroids, vitamin D analogs, retinoids, or tar. These treatments are applied directly to the skin and help reduce inflammation and scaling.
Phototherapy: Also known as light therapy, this treatment involves exposing the skin to ultraviolet (UV) light under controlled conditions. UVB and PUVA (psoralen plus UVA) are the two main types of phototherapy used to slow down cell turnover and reduce inflammation.
Systemic Medications: In cases of greater severity, healthcare providers may prescribe oral or injectable medications that specifically act on the immune system. These include methotrexate, cyclosporine, and biologics such as TNF-alpha inhibitors and IL-17 inhibitors.
Lifestyle Modifications: Making healthy lifestyle choices, such as maintaining a balanced diet, managing stress, avoiding smoking, and limiting alcohol consumption, can help manage psoriasis symptoms.
Topical Retinoids: Derived from vitamin A, retinoids are available in both topical and oral forms and help to reduce inflammation and slow down skin cell growth.
Biologics: These advanced medications target specific components of the immune system involved in psoriasis. They are often reserved for severe cases and have shown remarkable efficacy in symptom management.
Psoriasis Treatment Creams
Topical treatments are frequently the primary approach to address symptoms associated with psoriasis. Some commonly used psoriasis treatment creams include:
Corticosteroid Creams: These creams contain steroids that aid in alleviating inflammation and relieving itching. They come in various strengths, with higher strengths reserved for severe flare-ups.
Calcipotriene Cream: This cream contains a synthetic form of vitamin D and is used to slow down skin cell growth and reduce scaling
Coal Tar Preparations: Coal tar has been used for decades to treat psoriasis due to its ability to reduce scaling, itching, and inflammation.
Salicylic Acid Creams: These creams help remove scales, promoting the effectiveness of other treatments.
Cost of Psoriasis Treatment in India
The cost of psoriasis treatment in India can vary based on the type of treatment, severity of the condition, and the healthcare facility. Topical treatments and phototherapy are generally more affordable, while systemic medications and biologics can be more expensive.
On average, the cost of a month's supply of topical treatments can range from INR 200 to INR 1500. Phototherapy sessions might cost around INR 1000 to INR 3000 per session. Systemic medications and biologics can cost significantly more, ranging from INR 5000 to INR 50,000 per month or more.
The Emotional Impact
Psoriasis can harm mental and emotional health in addition to its physical side effects. The visible nature of the condition can lead to feelings of self-consciousness, embarrassment, and even depression. It's crucial for individuals with psoriasis to seek support from healthcare professionals, support groups, and loved ones to manage the emotional aspect of the disease.
Psoriasis is a complex and chronic skin disease with a significant impact on the lives of those who experience it. While there is no definitive cure, a multitude of treatment options are available to manage its symptoms effectively. Through ongoing research and advancements in medical science, we can hope for improved psoriasis treatments and a deeper understanding of the underlying causes of psoriasis. If you or someone you know is dealing with psoriasis, remember that seeking medical guidance and support is key to managing this condition and enhancing overall quality of life.
Frequently Asked Questions (Psoriasis)
Q. What is psoriasis?
A. Psoriasis is a chronic autoimmune skin disorder that leads to the rapid buildup of skin cells, resulting in red, scaly patches on the skin's surface. It is a non-contagious condition that can vary in severity and impact different parts of the body.
Q. What are the common psoriasis symptoms?
A. The common psoriasis symptoms include red patches covered with silvery-white scales, itching, discomfort, nail changes (pitting or separation), and joint pain (psoriatic arthritis). Inverse psoriasis can occur in skin folds, and the Koebner response can lead to psoriasis at sites of skin injury.
Q. Is psoriasis contagious?
A. No, psoriasis is not contagious. It cannot be spread through physical contact, like touching or sharing personal items.
Q. Is there a cure for psoriasis?
A. There is currently no cure for psoriasis, but various treatment options are available to manage symptoms and improve quality of life. Treatment aims to reduce inflammation, slow down skin cell growth, and alleviate discomfort.
Q. Are there any natural remedies for psoriasis?
A. While there is no definitive natural remedy for psoriasis, some individuals find relief through methods such as moisturizing, exposing skin to sunlight (in moderation), managing stress, and incorporating anti-inflammatory foods into their diet.
Q. Can psoriasis affect other parts of the body besides the skin?
A. Yes, some individuals with psoriasis may develop psoriatic arthritis, a condition that causes joint pain, stiffness, and swelling. This can affect various joints and lead to mobility issues if not properly managed.
Q. How is psoriatic arthritis diagnosed?
A. Diagnosis of psoriatic arthritis involves a combination of clinical evaluation, medical history, imaging tests (such as X-rays), and sometimes blood tests to rule out other conditions.
Q. Is there a link between psoriasis and other health conditions?
A. Psoriasis has been associated with an increased risk of other health conditions, including cardiovascular disease, diabetes, obesity, and certain autoimmune diseases. Regular medical check-ups and a healthy lifestyle are recommended to manage overall health.
Q. Can psoriasis develop in children?
A. Yes, psoriasis can develop in children and is known as pediatric psoriasis. It can present similarly to adult psoriasis but may require specialized treatment approaches suitable for children.